More about pharmacotherapy for depression
Adequate pharmacotherapy use
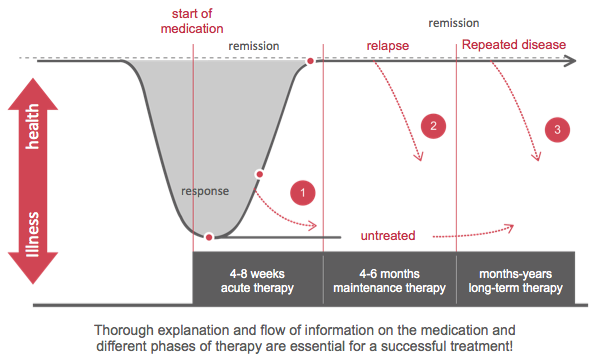
Pharmacotherapy for depression should consist of acute therapy up until the best clinical response or remission is achieved (usually 6-12 weeks) and continuation therapy for a further six months to prevent relapse. Sometimes, maintenance therapy will continue for months or years in case of recurrent or persistent disorders. Rates of relapse are about twice as high when antidepressant medication is discontinued before the end of the continuation phase so adherence is important, even if early improvement is achieved.
Most common antidepressant medication
There are different types of medication used in depression treatment. For the choice of the medication, several factors need to be considered by the doctor: e.g. predominant symptoms, previous experience, preference of the patient, as well as side effects. In this context, the distinction between unipolar or bipolar depression is crucial. Usually, this step takes place before you become involved as a pharmacist. The most common groups of medication commonly associated with depression treatment and their characteristics are:
Antidepressants:
- It is important to reassure patients that they are not addictive and not change personality;
- Patients should be advised that patience is necessary because there is a delay in onset of antidepressant action (about 2 - 4 weeks) while some side effects (e.g. nausea in SSRIs) occur at the start of the medication.
Sedatives/Tranquilizers:
- Can be used in addition to antidepressants for short periods only, e.g. during the first two weeks until the antidepressants start to work;
- Strongly associated with risk of addiction;
- Habituation (increasing doses to relieve symptoms) and withdrawal effects;
- Should be used temporarily in acute cruises to relieve suffering and anxiety, insomnia and eventually reduce suicide risk.
Neuroleptics:
- Traditionally used for schizophrenic disorders;
- Used for delusional depression (psychotic depression) mostly in combination with antidepressants;
- Some are also used in low dose as tranquilizers (e.g. ciamemazine, quetiapine) in depression and anxiety disorders
- No risk of addiction.
Anti-epileptics:
- Classically used for epilepsy, they have mood stabilising qualities;
- Recommended for bipolar depression and mania treatment and prevention.
Natural antidepressants:
- St. John's Wort is a hypericum perforatum extract substance, with a recommended dosage of about 500-800mg. The latency of its effect is three weeks, similar to synthetic antidepressants. The treating physician should be consulted about duration of treatment and parallel intake of other medication;
- There is no existing evidence base for the use of other purported natural antidepressants such as omega-3 fatty acids.
Mechanisms of antidepressant effects
The exact neurochemical dysfunction of depression is not known. Antidepressants appear to increase the availability of the neurotransmitters serotonin and noradrenalin in the synaptic cleft in some parts of the brain. However, at the same time, recent pre-clinical studies show that antidepressants consistently reduce the activity of neurons in the locus coeruleus in the brain stem where the noradrenergic neurons are located. Antidepressants also increase the availability of BDNF, a neurotrophin involved in neurogenesis and neuroplasticity.
Common side effects of antidepressants
Like all drugs, antidepressants have side effects. Every individual reacts differently and not every drug has the same side effects to the same degree. Many times patients experience secondary effects in the first week of antidepressant treatment: agitation or drowsiness, dry mouth, nausea, or ‘feeling peculiar’. Many of the side effects can be managed with simple diet and physical activity adjustments.
The desired antidepressant effect normally arises after two to six weeks of treatment, but the side effects often occur right from the beginning of the treatment. This can be very frustrating and may reduce adherence. As a pharmacist, you can let the patient know that this might happen and that such symptoms will subside. It is important to direct them not to discontinue the intake of the medication and to discuss their concerns with the physician in charge of treatment.
Les mécanismes des effets des antidépresseurs
Le dysfonctionnement neurochimique précis de la dépression n'est pas connu. Les antidépresseurs semblent augmenter la disponibilité des neurotransmetteurs sérotonine et noradrénaline dans la fente synaptique dans certaines parties du cerveau. En même temps, des études précliniques récentes ont montré que les antidépresseurs réduisent constamment l'activité des neurones dans le locus coeruleus du tronc cérébral, où se trouvent les neurones noradrénergiques. Les antidépresseurs augmentent également la disponibilité de BDNF dans le système limbique, une neurotrophine impliquée dans la neurogenèse et la neuroplasticité.
Effets secondaires courants des antidépresseurs
Comme tous les médicaments, les antidépresseurs ont des effets secondaires. Chaque individu réagit différemment et tous les médicaments n'ont pas les mêmes effets secondaires et au même niveau. Souvent les patients ressentent des effets secondaires pendant la première semaine du traitement aux antidépresseurs : de l'agitation ou de la somnolence, une sécheresse de la bouche, des nausées ou 'se sentir bizarre'. Beaucoup d'effets secondaires peuvent être gérés par des ajustements au niveau de l'alimentation et de l'activité physique.
L'effet antidépresseur désiré a normalement lieu après deux à six semaines de traitement, mais les effets secondaires apparaissent souvent dès le début du traitement. Ceci peut être frustrant et peut diminuer l'adhérence. En tant que pharmacien, vous pouvez avertir le patient que ceci peut arriver et que ces symptômes vont diminuer. Il est important de lui indiquer de ne pas interrompre la prise des médicaments et de parler de ses inquiétudes avec son médecin traitant.



